
Accounts receivable is often one of the most important areas of revenue cycle management as it represents potential money. In fact, A/R is considered an asset for that reason. The challenging part is that if A/R is not followed-up with quickly enough it can become a liability for the organization instead. Non-federal payers typically have timely filing/appeal limits between 120 – 180 days on average. When A/R ages beyond that it largely becomes uncollectable.
So, how do we improve performance with A/R collections? The first step is to identify and allocated A/R into buckets based on the date of service. Most of the industry defaults to A/R buckets that begin with ‘0 – 30’ days since the date of service.
Though these buckets served us well for many decades, they no longer support our analytical needs. The original buckets were designed to give time for claims to be transmitted to and from the insurance company by USPS®. Since the vast majority of our claims are now transmitted electronically, we can (and should) look at this information much sooner. A/R collection buckets fit us much better in today’s age of electronic transmissions and responses if we look at claims after 15 days instead of 30.
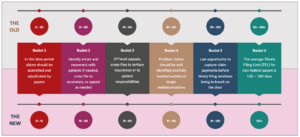
When we wait to review A/R we risk a lot:
- Timely filing/timely appeals windows can close.
- Patients with bad data in the system can be seen again before we know we need information from them.
- The revenue cycle velocity is lengthened which can reduce the days cash on hand.
In addition to shortening our A/R buckets we want to tackle other challenging areas of our A/R by asking the following questions of our teams:
- What are our current A/R balances?
- How are we grouping our A/R for review?
- Is this sufficient for our assessment needs long-term?
- What does our data tell us our collection rate is for each bucket?
- Where do we have opportunities in the future to prevent rising A/R?
- How do we define ‘optimal’ in terms of total balance by bucket as well as collection rate?
Lastly, run reports on your underpaid claims. These claims may still be sitting in /R and if they represent true underpayments then the team needs to investigate why they occurred. Is there a quality- or value-based penalty in play? Did the payer reimburse you at the wrong rate? Do you need to invoice the patient for a different amount than what was originally posted?
Asking these questions and identifying the answers will help you create a strategy around your A/R that prevents claims from aging while improving collection rates.
For additional resources on A/R give us a shout, we are here to support.
Taya Gordon, MBA, FACMPE, CMOM
LinkedIn: https://www.linkedin.com/in/tayagordon/
Twitter: https://twitter.com/tayamoheiser

